
Cancer Survivorship Optimization
Summary
How might we create a more equitable and inclusive experience for all cancer survivorship patients at Cincinnati Children's Hospital Medical Center?
Role
Project Lead / Researcher
Client
Cincinnati Children’s Hospital
Skills
User Interviews, UX Research, Project Management
Background & Objectives
Background
The Cancer Survivorship Center provides lifelong care for pediatric cancer survivors, yet disparities in patient retention—particularly across racial and ethnic groups—revealed gaps in the experience.
Objective
Identify and address inequities in the survivorship experience to support long-term engagement and continuity of care.
My Role
- Helped define research direction across a year-long engagement
- Conducted and synthesized qualitative interviews
- Led journey mapping and persona development
- Translated findings into opportunities for equitable design
Research Focus
This project focused on understanding how patients, especially patients of color, experience survivorship care over time, and what barriers impact their continued engagement.
This project is ongoing at the Live Well Collaborative and I was happy to participate in a year of this project.
Process
- Foundational Research → Understanding the System
We began with background research and stakeholder interviews to understand:
- The structure of the Survivorship Center
- Clinical workflows and staff perspectives
- Existing assumptions about patient behavior
This phase helped us identify early gaps between provider expectations and patient realities.
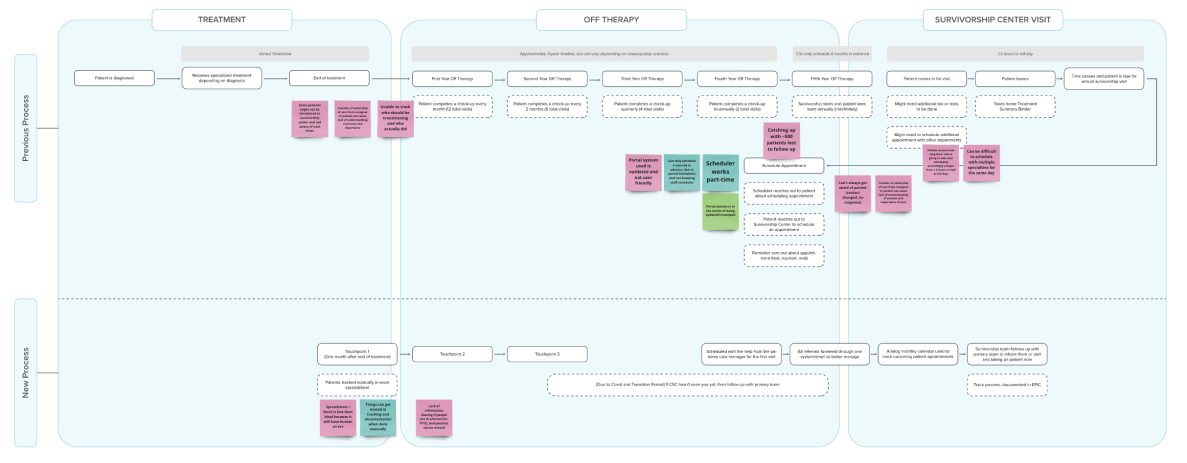
- Stakeholder & Patient Interviews → Challenging Assumptions
Deeper Understanding
We interviewed patients and staff to correct some misconceptions we had about the process.
Method:
- Semi-structured interviews to allow for personal storytelling
- Focus on emotional, logistical, and behavioral aspects of care
- Iterative questioning to probe initial assumptions
Key learning: Early research revealed that some of our initial assumptions about patient disengagement were incomplete or incorrect, prompting a shift in research direction.
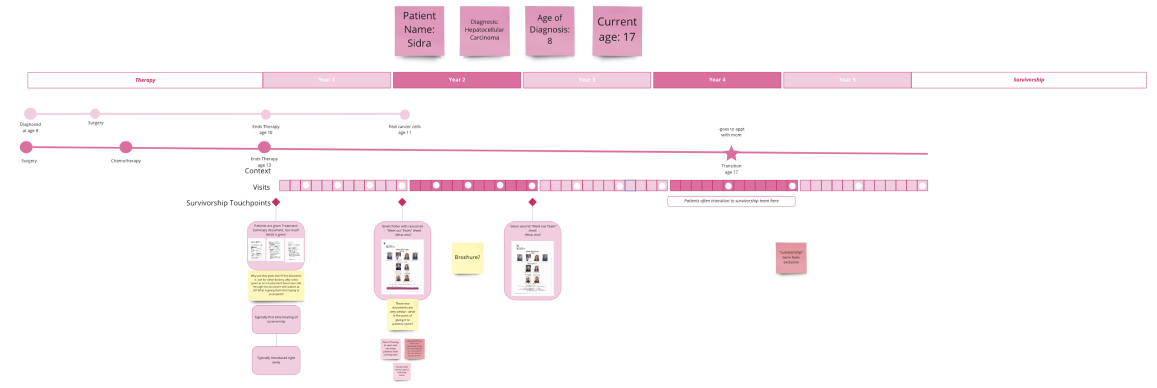
- Journey Mapping → Identifying Drop-Off Points
We mapped end-to-end patient journeys from treatment completion through survivorship care.
This helped us identify:
- Key transition moments (e.g., aging out of pediatric care, starting college)
- Points where patients disengage
- Emotional highs and lows within the experience
- Equity-Focused Research → Centering Underrepresented Voices
Focus Shift
In later phases, we focused specifically on interviewing patients of color to better understand differences in experience.
We examined:
- Trust in healthcare systems
- Emotional associations with returning to the hospital
- External life pressures (school, work, family)
- Language and framing of “survivorship”
This ensured our insights reflected diverse lived experiences, not just majority perspectives
- Synthesis → From Stories to Patterns
We synthesized interviews and journey maps into key themes:
Emotional AvoidancePatients associate the hospital with trauma, leading to delayed or skipped follow-ups
Life TransitionsMajor life changes (college, independence) disrupt care routines
Motivation vs. FrictionPatients often intend to return but lack urgency or support
Language & ClarityTerms like “survivorship” are not always intuitive or meaningful
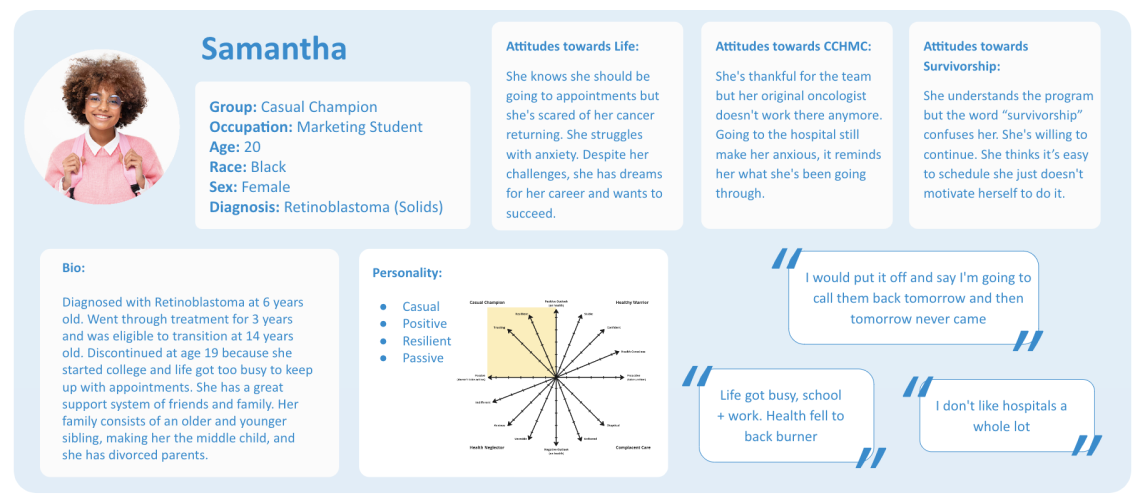
- Persona Development → Making Insights Actionable
We developed personas to represent key patient segments, grounding them in real behaviors and attitudes.
These personas highlighted variations in motivation and support systems, differences in emotional readiness to re-engage with care, and equity-related gaps in experience and access.
Impact
Challenging Assumptions
Revealed key drivers of patient disengagement beyond surface-level assumptions
Center Equity
Prioritize underrepresented patient experiences
Powerful Catalyst
Provide a research-backed foundation for future solution development
Cancer Survivorship Optimization

Summary
How might we create a more equitable and inclusive experience for all cancer survivorship patients at Cincinnati Children's Hospital Medical Center?
Role
Project Lead / Researcher
Client
Cincinnati Children’s Hospital
Skills
User Interviews, UX Research, Project Management
Background & Objectives
Background
The Cancer Survivorship Center provides lifelong care for pediatric cancer survivors, yet disparities in patient retention—particularly across racial and ethnic groups—revealed gaps in the experience.
Objective
Identify and address inequities in the survivorship experience to support long-term engagement and continuity of care.
My Role
- Helped define research direction across a year-long engagement
- Conducted and synthesized qualitative interviews
- Led journey mapping and persona development
- Translated findings into opportunities for equitable design
Research Focus
This project focused on understanding how patients, especially patients of color, experience survivorship care over time, and what barriers impact their continued engagement.
This project is ongoing at the Live Well Collaborative and I was happy to participate in a year of this project.
Process
- Foundational Research → Understanding the System
We began with background research and stakeholder interviews to understand:
- The structure of the Survivorship Center
- Clinical workflows and staff perspectives
- Existing assumptions about patient behavior
This phase helped us identify early gaps between provider expectations and patient realities.

- Stakeholder & Patient Interviews → Challenging Assumptions
Deeper Understanding
We interviewed patients and staff to correct some misconceptions we had about the process.
Method
- Semi-structured interviews to allow for personal storytelling
- Focus on emotional, logistical, and behavioral aspects of care
- Iterative questioning to probe initial assumptions
Key learning
Early research revealed that some of our initial assumptions about patient disengagement were incomplete or incorrect, prompting a shift in research direction.

- Journey Mapping → Identifying Drop-Off Points
We mapped end-to-end patient journeys from treatment completion through survivorship care.
This helped us identify:
- Key transition moments (e.g., aging out of pediatric care, starting college)
- Points where patients disengage
- Emotional highs and lows within the experience
- Equity-Focused Research → Centering Underrepresented Voices
Focus Shift
In later phases, we focused specifically on interviewing patients of color to better understand differences in experience.
We examined:
- Trust in healthcare systems
- Emotional associations with returning to the hospital
- External life pressures (school, work, family)
- Language and framing of “survivorship”
This ensured our insights reflected diverse lived experiences, not just majority perspectives
- Synthesis → From Stories to Patterns
We synthesized interviews and journey maps into key themes:
Emotional AvoidancePatients associate the hospital with trauma, leading to delayed or skipped follow-ups
Life TransitionsMajor life changes (college, independence) disrupt care routines
Motivation vs. FrictionPatients often intend to return but lack urgency or support
Language & ClarityTerms like “survivorship” are not always intuitive or meaningful
- Persona Development → Making Insights Actionable
We developed personas to represent key patient segments, grounding them in real behaviors and attitudes.
These personas highlighted variations in motivation and support systems, differences in emotional readiness to re-engage with care, and equity-related gaps in experience and access.

Impact
Challenging Assumptions
Revealed key drivers of patient disengagement beyond surface-level assumptions
Center Equity
Prioritize underrepresented patient experiences
Powerful Catalyst
Provide a research-backed foundation for future solution development